
Severe pain during the procedure usually results from the needle coming into contact with the highly innervated cartilaginous surfaces. 
The Patient Complains of Severe Pain During the Procedure. The patient is warned to avoid forceful activity on the joint while it is anesthetized. The skin is cleansed, and a bandage is is applied over the needle-puncture site. After injection of the medication, the needle and syringe are withdrawn. Alternately, methylprednisolone (Depo-Medrol, 40 mg per mL), 1 mL, mixed with 3 to 5 mL of 1 percent lidocaine can be used. A syringe filled with corticosteroid medication can then be attached to the needle.įor injection, use betamethasone (Celestone, 6 mg per mL), 1 mL, mixed with 3 to 5 mL of 1 percent lidocaine. Care should be taken not to touch the needle tip against the joint surfaces when removing the syringe. With the needle stabilized with the hemostat, the syringe can be disconnected and the fluid sent for studies. Once the syringe has filled, a hemostat can be placed on the hub of the needle. Using the nondominant hand to compress the opposite side of the joint or the patella may aid in arthrocentesis. 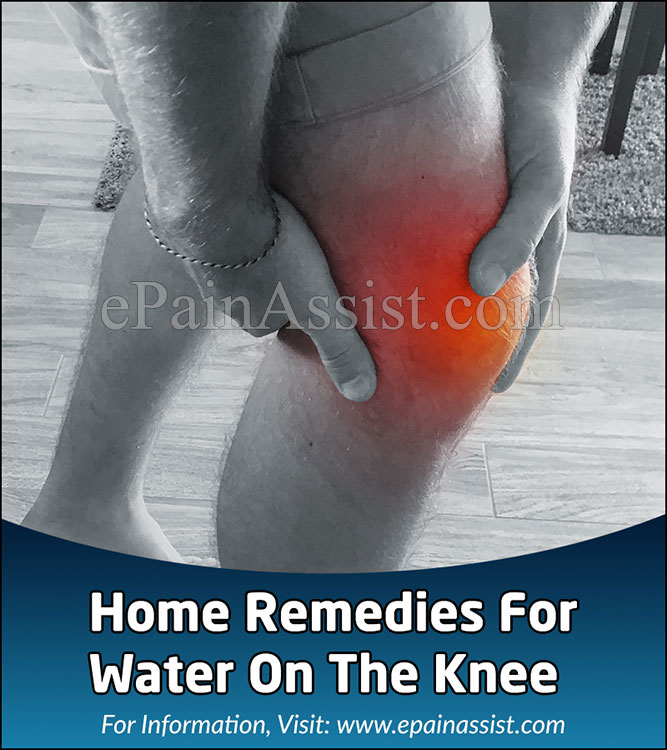
Once the needle has been inserted 1 to ¼ inches, aspiration is performed, and the syringe should fill with fluid. The needle is directed at a 45-degree angle distally and 45 degrees into the knee, tilted below the patella ( Figure 1). Some physicians administer lidocaine (Xylocaine) into the skin, but stretching the pain fibers in the skin with the nondominant hand can also reduce needle-insertion discomfort. The needle is inserted through stretched skin. A 21-gauge, 1-inch needle is attached to a 5- to 20-mL syringe, depending on the anticipated amount of fluid present for removal. The physician should be gloved, although there is no consensus as to whether sterile gloves must be used. The skin is washed with povidone-iodine solution. 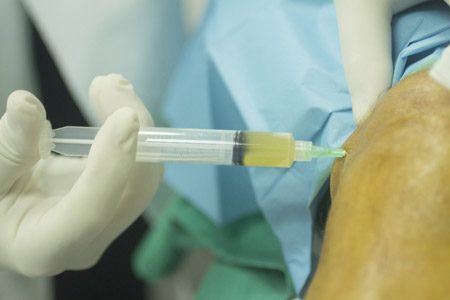
This location provides the most direct access to the synovium. The skin is marked with a pen, one fingerbreadth above and one fingerbreadth lateral to this site. The superior lateral aspect of the patella is palpated. The knee is examined to determine the amount of joint fluid present and to check for overlying cellulitis or coexisting pathology in the joint or surrounding tissues. Some physicians prefer the medial approach for smaller effusions, but the lateral approach will be discussed here. The patient is supine on the table with the knee extended (some physicians prefer that the knee be bent to 90 degrees). Anti-inflammatory medications may prove beneficial in reducing joint inflammation and fluid accumulations. Large effusions can recur and may require repeat aspiration. Contraindications include bacteremia, inaccessible joints, joint prosthesis, and overlying infection in the soft tissue. Among the indications for arthrocentesis are crystal-induced arthropathy, hemarthrosis, unexplained joint effusion, and symptomatic relief of a large effusion. Local corticosteroid injections can provide significant relief and often ameliorate acute exacerbations of knee osteoarthritis associated with significant effusions. Once the needle has been inserted 1 to 1½ inches, aspiration aided by local compression is performed. One approach involves insertion of a needle 1 cm above and 1 cm lateral to the superior lateral aspect of the patella at a 45-degree angle. The knee joint is the most common and the easiest joint for the physician to aspirate. Knee joint aspiration and injection are performed to aid in diagnosis and treatment of knee joint diseases.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
